Symmetrical Peripheral Gangrene Caused by High Dose Vasopressors: Two Case Reports
Article information
Abstract
Vasopressors, such as norepinephrine, dopamine and vasopressin are commonly used treatments for the major circulatory failure. Despite of its favorable purpose, these agents induce adverse effects. Symmetrical peripheral gangrene (SPG) is a rare but severe complication characterized by ischemic changes of two or more extremities without larger vessel occlusion. Recently, we experienced 2 cases of SPG caused by vasopressor infusion that progressed in different courses. Both cases showed severe ischemic changes in every digit but only the second case aggravated to lower limb surface necrosis. Treatments should be based on the complication of each vasopressor and be individualized by each patient. Further studies concerning maximal dose of each vasopressor are required.
Introduction
According to Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock, norepinephrine is the first choice vasopressor which stimulate both alpha- and beta-receptors [1]. In therapeutic dose, its alpha-1 effect predominates, inducing peripheral vasoconstriction. It is advised to add either vasopressin or epinephrine to raise mean arterial pressure (MAP) to the target or adding just vasopressin to reduce norepinephrine dosage. Dopamine is limited to when norepinephrine is not available or with highly selected patients [2]. Since the maximal dose of these vasopressors is controversial worldwide, adverse effects, such as SPG are become important issue in wound management area. We have treated 2 cases of SPG caused by high dose vasopressors which progressed in different courses. Treatments should be based on the clinical features of each vasopressor and be individualized by each patient.
Case
Case 1
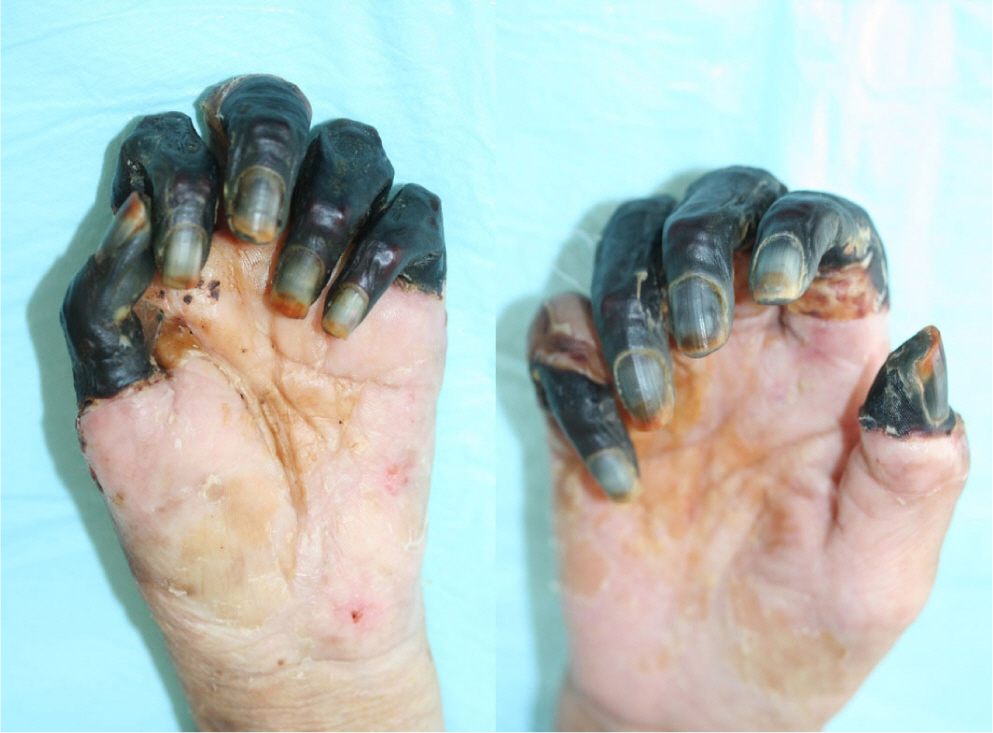
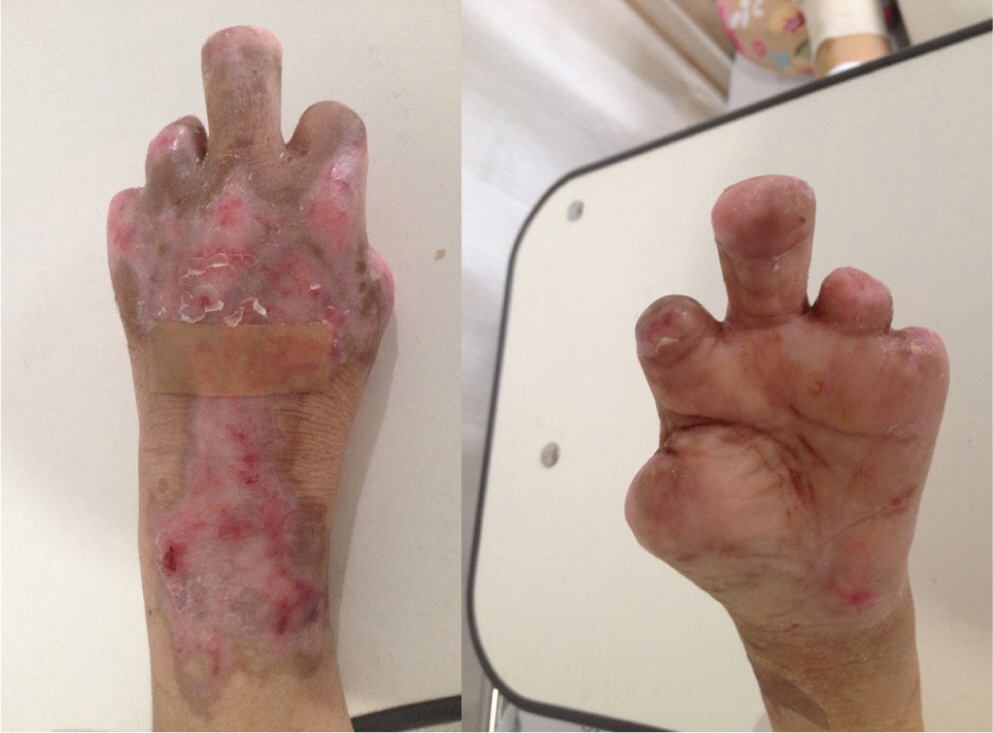
A 60-year-old female patient without any specific history, presented to emergency department with mental decrease. Following examination revealed subarachnoid hemorrhage with ruptured aneurysm and she underwent emergency aneurysm clipping. After the operation, she was transferred to the intensive care unit (ICU) and started on dopamine (10−20 µg/kg/min) and norepinephrine (0.3 µg/kg/min). In order to maintain MAP, both vasopressors were increased steadily and bilateral necrosis of all digits were observed (Fig. 1). All agents were tapered and discontinued since hospital day 20. Gangrenous finger tips were amputated and no further ischemic changes were seen afterwards (Fig. 2).
Case 2
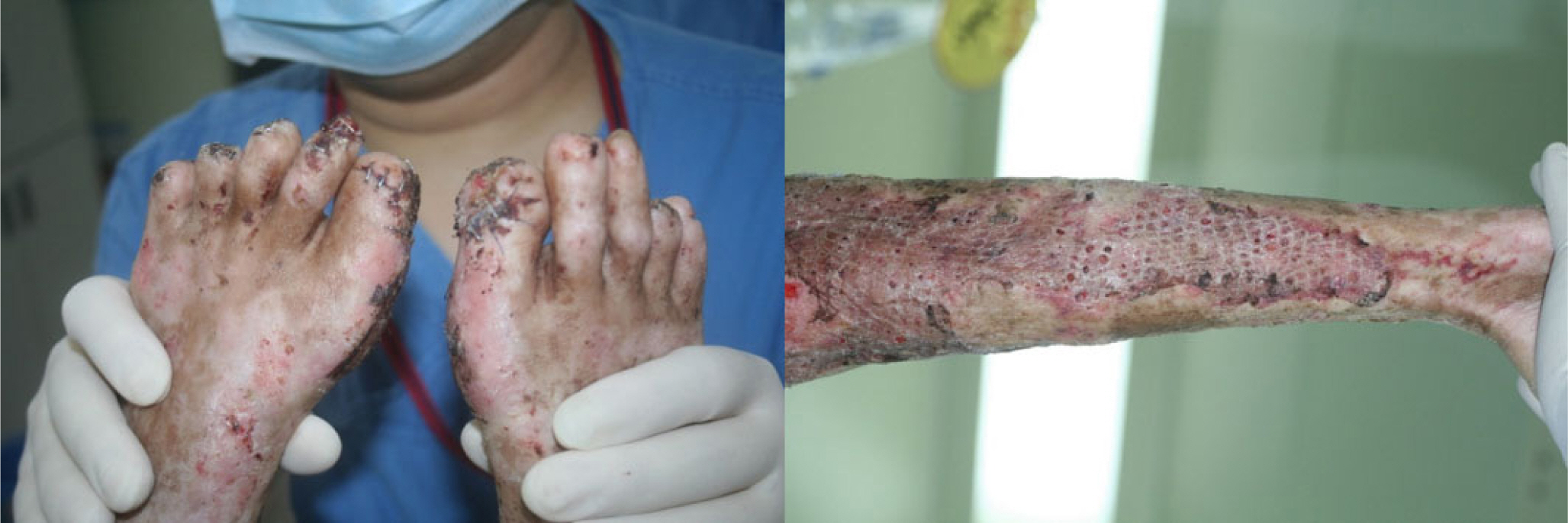
A 34-year-old female with cervical cancer visited emergency department with fever after several cycles of chemotherapy. Since her initial status was revealed as septic shock due to urinary tract infection, dopamine (10−20 µg/kg/min), vasopressin (0.03 U/min) and norepinephrine (3.0 µg/kg/min) were started immediately. Even though she recovered from initial condition, ischemic change of all digits and whole body color change with skin necrosis including thigh and lower leg surfaces were unavoidable (Fig. 3). Split-thickness skin graft following surgical debridement was performed on the surface of lower extremities and several toes were partially amputated (Fig. 4).

Pre-operative view of case 2. Not only both toe tips but also both thigh and lower leg surfaces were affected.
Discussion
SPG is uncommon condition usually caused by disseminated intravascular coagulation (DIC), hemodynamic compromise and sepsis [3,4]. In addition, the use of vasopressors may create the spasm of peripheral vessels and aggravate microcirculation problems simultaneously as in our cases [5]. However, according to Kingston and Mackey, SPG can be induced by other mechanisms such as direct vascular occlusion by bacteria, immune complex formation and emboli from endocarditis [6].
Meanwhile, clinical appearances of ischemic necrosis in each case were different. In case 1, gangrene occurred on all of her digital tips while thigh and lower leg surfaces were also involved in case 2. This is probably related to vasopressors used in each case; norepinephrine and dopamine in case 1 while norepinephrine, dopamine and vasopressin in case 2. According to previous reports, target receptors of vasopressin are located in smooth muscles of blood vessels which distributed mainly in splanchnic and skin circulation [7]. Therefore, wider surfaces of thigh and lower leg in case 2 might be affected by vasopressin. Moreover, it is worth debate that the initial dosage of norepinephrine in case 2 were 10 times higher than case 1.
Unlike general understanding over cardiovascular condition based on age, clinical course of case 2 was beyond our estimation. More extended forms of SPG were observed in younger age. Additionally, the aforementioned risk factors were not observed in case 1, but several predisposing factors, such as septic shock and DIC components were revealed by lab examination in case 2. Therefore, we can assume that current cardiovascular condition, not simply demographic data, is also an important factor causing different course of SPG along with vasopressors.
No specific treatments were indicated to prevent or reverse SPG. The treatment priority is the underlying condition, which requires fluid resuscitation, antibiotics, vasopressor therapy and ventilator. Therefore, SPG is typically not treated immediately [8]. Early recognition and proper management of SPG are necessary to avoid devastating results; amputation [5]. Supportive treatments that might be helpful, include sympathetic blockade, intravenous nitroprusside therapy, topical nitroglycerine ointment and intravenous infusion of prostaglandin are have been reported but these interventions are lack of evidence [9].
Approximately, more than half of the patients recover from SPG require amputation of the affected limb [4]. Amputation should be considered only after the patient’s condition improved and the gangrenous areas become demarcated [8]. However, many skin flaps are currently available and free flaps can be particularly effective for salvaging limbs [10].
Using vasopressors in septic condition is inevitable [5,8]. However, there are no consensus or guidelines for using high dose vasopressors established and it is supported by that the most common reason for ICU physicians to withhold or withdraw vasopressor administration was only a lack of response to maximal therapy [11]. Reyes et al. [12] reported that appropriate dosage of intravenous vasopressors should be individualized according to age, body mass index, MAP and clinical status of the patient.
To the best of our knowledge, there was no single report directly comparing clinical results of SPG progressed by each vasopressor. We report these cases to highlight the clinical features of SPG according to each vasopressor and to warn physicians to use vasopressors with extra-caution. Further studies should be focus on establishing the guidelines for individualized dosage of vasopressors and for distinguished treatment based on each vasopressor.
Notes
No potential conflict of interest relevant to this article was reported.