Introduction
Wound bed preparation refers not only to the removal of non-viable, damaged, or infected tissue, but also the maintenance of optimal wound conditions in terms of inflammatory cytokine and proteinase activity, moisture balance, the proper margin of the wound, and a low bacterial burden.
Early eschar removal could lead to a significant reduction in bacterial colonization, bacterial count, and infection rate [1,2]. Eschar removal shortens the inflammatory state by reducing the inflammatory cytokines and metalloproteinases that cause chronic wound inflammation [3]. Therefore, early eschar removal is considered an important step for improving the aesthetic and functional outcomes of burn treatment.
Several trials have investigated the timing and most accurate method of debridement for eschar removal. Other than the classical surgical technique, various other techniques have been attempted, including acids, proteolytic enzymes of bacterial or plant origin, collagenase-based gels, hydro-surgery, maggot therapy, and lasers [4,5]. Of these techniques, enzymatic debridement is regarded as a compelling method to dissolve eschars in burn wounds, mainly due to its potential for selective and safe eschar removal. It only affects the injured tissue (i.e., the eschar), while preserving the uninjured dermis and thereby reducing blood loss [4,6,7].
Based on increasing evidence of its safety and efficacy, Nexobrid (MediWound, Yavne, Israel), a mixture of proteolytic enzymes enriched in bromelain derived from pineapple stems, has become an effective and useful debridement tool for burn treatment as an alternative to surgical eschar removal [4,6-10].
The aim of this case report is to introduce Nexobrid, which is new to the Korean market, and to present our experiences with Nexobrid as a bromelain-based enzymatic debridement material. The report also intends to inform of a new enzyme therapy, allowing for comparison with existing methods in terms of the effectiveness of eschar removal.
Case
We treated seven scalding burn patients with Nexobrid (Table 1). All burn wounds were evaluated and treated by one experienced burn surgeon (HSJ). The study was approved by the Institutional Review Board of Hanil General Hospital (IRB No. HGH-2021-OTH-010) and performed in accordance with the principles of the Declaration of Helsinki. Written informed consents were obtained.
Care of the wound bed prior to debridement
Pre-debridement and debridement management were conducted in a routine manner according to the manufacturer’s instructions.
The wounds were cleaned with normal saline, blisters and keratin debris were removed, and the burned area was covered with a 3- to 5-mm-thick layer of topical anesthesia cream (EMLA; AstraZeneca, London, UK) for a minimum of 2 hours.
Enzymatic debridement
An additional analgesic agent was administered 10–15 minutes prior to application of Nexobrid, with additional analgesic administration during Nexobrid application upon the patient’s request.
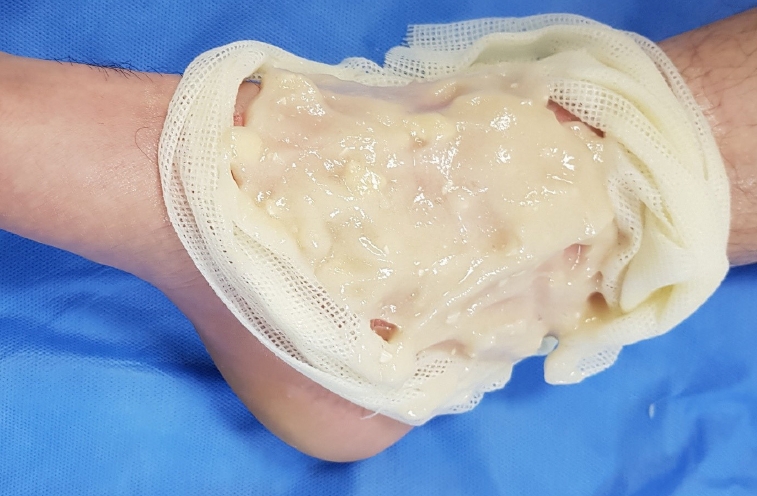
The burned wounds were covered with a 1- to 3-mm-thick layer of a mixture of lyophilized powder and vehicle gel (2 g of enzyme in 20 g of gel to cover 10×10 cm). The area was then sealed with a polyurethane occlusive sheet (Perme Roll; Nitto, Tokyo, Japan) that was separated from the surrounding normal skin with a sterile vaseline sheet (Bactigras; Smith & Nephew, Watford, UK) and dressed with mild compressive dressing for a period of 4 hours (Fig. 1). Four hours after application, the dressing was removed, and the remaining materials were cleaned out and cleaned gently with normal saline. The wounds were then further dressed with antibacterial ointment and foam material (Biatain Ibu; Coloplast, Peterborough, UK).
Care of the debrided wound
The wounds were reassessed on the next day, focusing on whether or not the eschar was removed (≥90%). When debridement was considered complete in terms of eschar removal and there was enough residual viable dermis with dermal pinpoint bleeding, the standard treatment was performed to promote healing. In cases with a full-thickness defect or remnant eschar, the wound was autografted as early as possible.
Cases
Case 1
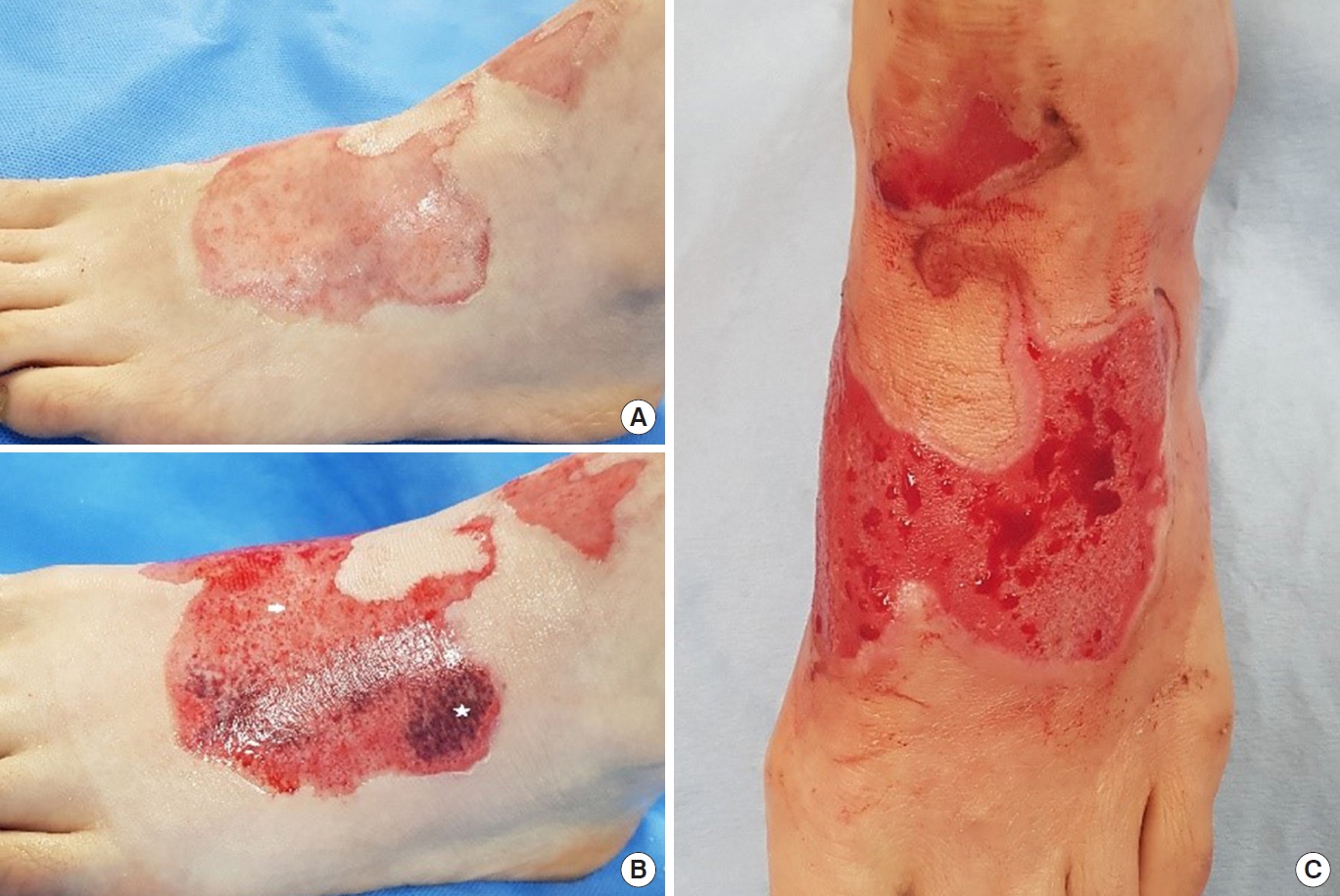
A 46-year-old woman was injured by hot soup spilling onto the anteromedial aspect of her left foot at work. On the day of admission, the initial wound state involved a ruptured blister that was removed. The wound bed had a pale white and mottled color, was more edematous than the surrounding normal skin, and had a blanched, bloodless surface (Fig. 2A). On the second day after the injury, we performed enzymatic debridement and re-evaluated the depth of the burn wound. The enzymatically debrided wound bed had a pink to red color and there was pinpoint punctate bleeding mixed with whitish collagen stroma. A red circular pattern was observed in the dermis, implying that the deeper dermis was affected (Fig. 2B). We assessed the wound as mostly involving partial-thickness burns. We therefore provided standard dressing using antibacterial ointment and foam, expecting spontaneous epithelialization. On the fifth day after debridement, the wound bed had a uniform pink color with bloody areas, and the edge of the wound was epithelized (Fig. 2C).
Case 2
A 41-year-old man was burned by ramen on the medial aspect of his right foot. The wound bed was initially bloodless, pale in color, and mildly depressed compared to the surrounding normal skin (Fig. 3A). On the third day after the injury, we treated the wound using enzymatic debridement. The wound bed showed a uniform white color with pinpoint punctate bleeding (Fig. 3B). Based on the bleeding pattern, we assessed the wound as a partial-thickness burn and treated the patient with the standard method.
Case 3
A 45-year-old man was burned by hot water on the dorsum of his right foot. He was admitted on the seventh day after the injury. The wound had a dry, white-leathery eschar and a dirty scab (Fig. 4A), on which Nexobrid was promptly applied on admission. The enzymatically debrided wound showed a bloodless mottled bed, visible clotted vessels in the dermis, and eschar remnants (Fig. 4B). We judged the entire wound to be a full-thickness burn and performed skin grafting.
Discussion
Burn wounds are differentiated from other traumatic or inflammatory wounds by the presence of a necrotic eschar formed by damaged proteins, inducing an inflammatory reaction that results in delayed epithelialization and increased risks of infection and subsequent scarring.
Autolytic debridement of partial or small eschars in deep second- or third-degree burns can be achieved through conservative management during a course of up to 2 weeks in selected cases. However, this prolonged process can result in inflammation or infection that may worsen the depth of the burn by transforming the zone of hyperemia and stasis into a zone of necrosis and by facilitating the development of granulation tissue, which leads to deforming scars.
Surgical debridement has been considered a standard procedure to promote healing and prevent scarring. However, due to poor selectivity, surgical excision often sacrifices viable skin together with necrotic tissue and results in significant blood loss. The loss of viable dermis reduces the ability of partialthickness and mixed-depth burns to heal spontaneously, increasing the surgical risk and the likelihood of scarring [7].
Research on nonoperative debridement of burns has aimed at effectively promoting autolysis. Various substances such as enzymes of plant origin and acids and proteolytic enzymes of bacterial origin have been examined since the Second World War. A vegetable pepsin (papain) was found to be of limited utility, with no significant difference from conventional autolysis. Acids have the disadvantage of risk of severe systemic acidosis and the potential to damage normal skin. Meanwhile, collagenase is limited by its slow action and poor efficacy, and enzymes from bacteria pose a risk of systemic bacteremia and wound infection [3,5].
The effectiveness of enzymatic substances based on bromelain (Nexobrid) has been recognized in recent years. These preparations selectively remove eschars without harming viable tissue and preserve viable dermis or subdermal tissue, which can promote spontaneous epithelialization and reduce bleeding.
Nexobrid consists of a lyophilized, partially purified proteolytic enzyme mixture derived from bromelain extracted from pineapple plant stems. It has the ability to selectively dissolve denatured proteins in burn wounds. As a result, Nexobrid reduces inflammation, inducing less granulation tissue formation and scarring and leaves sufficient dermal remnants to promote spontaneous healing [6-9]. Furthermore, rapid regeneration within 21 days can prevent excessive formation of scars, possible resulting in better cosmetic outcomes [10]. Acute burns display a wide range of depths, which are difficult to accurately measure. Due to the heterogeneity of acute burns and the difficulty in assessing their depth, early diagnosisbased treatment is often impossible. In contrast, enzymatic debridement enables an exact diagnosis of the burn depth and helps to reduce the autografted area in mixed-degree burns. This technique also enables eschar removal on even irregular anatomical areas and reduces elevated interstitial compartment pressure. Therefore, enzymatic debridement can be effective for burns of the face and hand [9,11]. Since it can promote wound healing prior to excessive scar formation, it is particularly suitable for the face and hands where cosmetic or motor functions are particularly important.
Nonetheless, Nexobrid does have its limitations. Patients complain of moderate to severe pain while applying Nexobrid. Topical anesthesia, regional block, or analgesics are therefore necessary as pre-treatment. In addition, old, desiccated, and thick eschars may not dissolve completely. Furthermore, according to the literature, silver sulfadiazine or povidone-iodine saturated eschars are also hard to remove [6-8].
According to our experience and review of literature review, Nexobrid could be an effective debridement agent for burn treatment because of its selectivity and efficiency. It helps early diagnoses and creates a clean wound bed in burns with good prognosis for wound healing and scarring. The shortcoming of this paper is that the authors were not able to apply this drug to a variety of patients because Nexobrid was only made available in Korea recently. As the authors’ results cannot be compared with the reports from Europe, it is not possible to establish a definitive method of use or to produce definite conclusion. This highlights the need for further investigation into the use of Nexobrid.